‘Loneliest road I’ve walked’ – KZN mom’s sunken chest put pressure on her lungs and heart
A KZN mother’s journey through Pectus Excavatum that placed dangerous pressure on her lungs and heart — and how surgery changed everything.
A KZN mother’s journey through Pectus Excavatum that placed dangerous pressure on her lungs and heart — and how surgery changed everything.
Justin Reichlin spent his life hiding a sunken chest — until a groundbreaking South African-invented procedure finally performed locally changed everything. He was only the third patient to benefit.
Chest wall deformities are far more than cosmetic concerns. In South Africa, pioneers like Dr. Ivan Schewitz have transformed care with minimally invasive techniques, changing lives across the continent.
Chest wall deformities are fundamentally congenital conditions arising from an overgrowth or growth disturbance of the costal cartilage that connects the ribs to the sternum. This cartilage growth exerts mechanical force on the sternum, resulting in either a posterior displacement, known as pectus excavatum, or an anterior protrusion, known as pectus carinatum. While these conditions may be present at birth, they frequently remain subtle until the onset of puberty, when rapid skeletal growth exacerbates the deformity and makes it clinically prominent.
The distribution of these conditions across the population reveals a persistent male predominance, with males being affected three to five times more frequently than females. Pectus excavatum, often termed “funnel chest,” is significantly more common, accounting for 65% to 95% of all chest wall anomalies. Pectus carinatum, or “pigeon chest,” while less frequent, presents its own set of distinct clinical challenges, particularly regarding the flexibility of the chest wall as the child approaches maturity.
| Epidemiological Feature | Pectus Excavatum (Sunken) | Pectus Carinatum (Protruding) |
|---|---|---|
| Common Clinical Names | Funnel Chest, Sunken Chest, Hallowed Breast | Pigeon Chest, Chicken Breast, Keeled Chest |
| Incidence (Live Births) | 1 in 300 to 1 in 400 | 1 in 1,000 to 1 in 1,500 |
| Gender Predisposition | Highly prevalent in males (3:1 to 5:1) | Highly prevalent in males (4:1) |
| Common Genetic Links | Marfan, Ehlers-Danlos, Scoliosis | Marfan, Rickets, Cardiac Abnormalities |
| Typical Discovery Age | Infancy or Puberty (Growth Spurt) | Late Childhood or Puberty |
| Frequency Among Deformities | ~85% of cases | ~15% of cases |
The prevalence rates suggest that while these conditions are relatively common, they remain underrecognized in general pediatric screening and sports cardiology. This lack of awareness often leads to delayed diagnosis, which can be detrimental as the ideal window for non-surgical or minimally invasive interventions begins to close during late adolescence.

Dr. Ivan Schewitz has emerged as the definitive authority on pectus deformities within South Africa, bringing decades of specialized experience to a field that was previously dominated by invasive, radical surgical approaches. Based at the Pectus Clinic in Midrand, Gauteng, Dr. Schewitz’s career is characterized by a commitment to innovation and the integration of international best practices into the local medical framework.
After qualifying as a Cardiothoracic Surgeon in 1985, Dr. Schewitz dedicated himself to refining thoracic procedures, eventually becoming the surgeon who introduced the minimally invasive repair of pectus excavatum “the Nuss procedure” to South Africa. His influence extends beyond the operating room; he serves as a consultant for several prestigious institutions, including the University of Pretoria and the University of Cape Town, and is a council member of the South African Thoracic Society.
| Professional Profile | Details |
|---|---|
| Professional Profile: Dr. Ivan Schewitz | https://www.schewitz.com/ |
| Primary Specialisation | Cardiothoracic Surgery, Pectus Deformity Correction |
| Key Innovations Introduced | Nuss Procedure (PE), VATS, 3D Bracing (PC) |
| Clinic Location | Room 202, Netcare Waterfall City Hospital, Midrand |
| Affiliations | Chest Wall International Group (CWIG), SA Thoracic Society, Pan African Thoracic Society, European Society of Thoracic Surgery |
| Academic Roles | Honorary Consultant at UP and UCT; VATS Workshop Director |
| Hospital Access | Netcare Waterfall |
Dr. Schewitz’s work has fundamentally shifted the perception of chest wall deformities from being viewed as “cosmetic” issues to being understood as serious medical concerns with profound implications for cardiac and respiratory health. His presentation of over 40 cardiothoracic papers, many specifically focused on pectus correction, underscores his role as a thought leader in the global thoracic community.
Pectus excavatum is defined by an inward depression of the sternum, which can range from a mild, barely perceptible dip to a severe indentation that displaces the heart and compresses the lungs. The physiological consequences of this condition are often underestimated in the medical community. When the sternum is significantly depressed, it physically limits the space available in the thoracic cavity, forcing the heart – specifically the right ventricle, to become compressed and shifted toward the left side of the chest.
This compression is not merely an anatomical curiosity; it has measurable impacts on cardiovascular performance. Research has demonstrated that individuals with severe pectus excavatum may experience a significant reduction in cardiac output, particularly during exercise. This occurs because the heart is unable to fill completely during its relaxation phase (diastolic filling), leading to a lower stroke volume. For the adolescent patient, this manifests as exercise intolerance, premature fatigue, and shortness of breath that is often disproportionate to their physical conditioning.
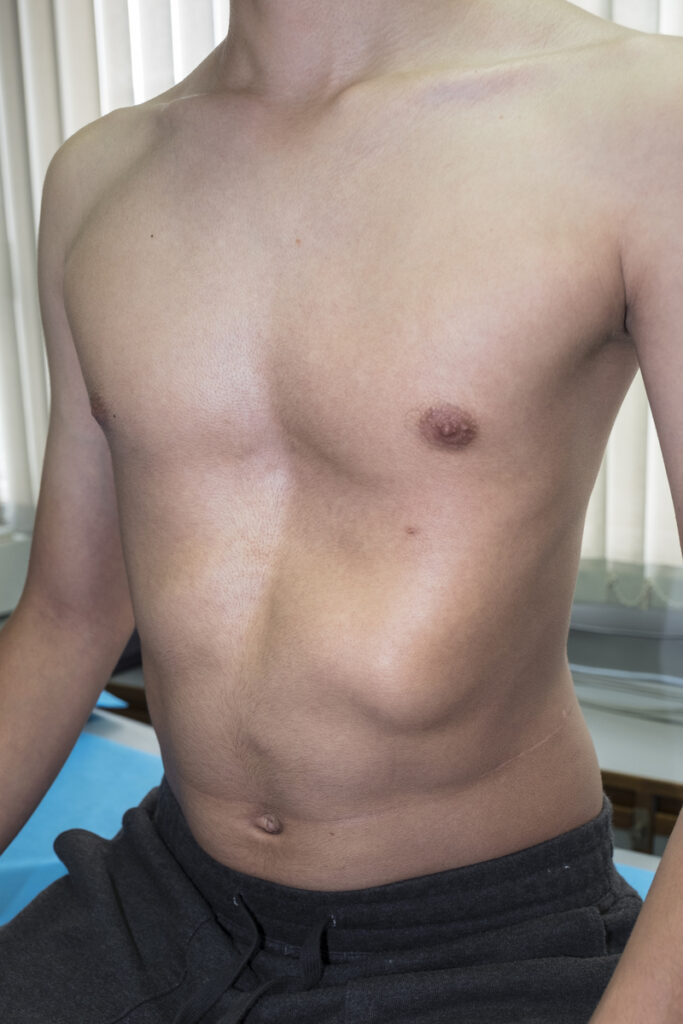
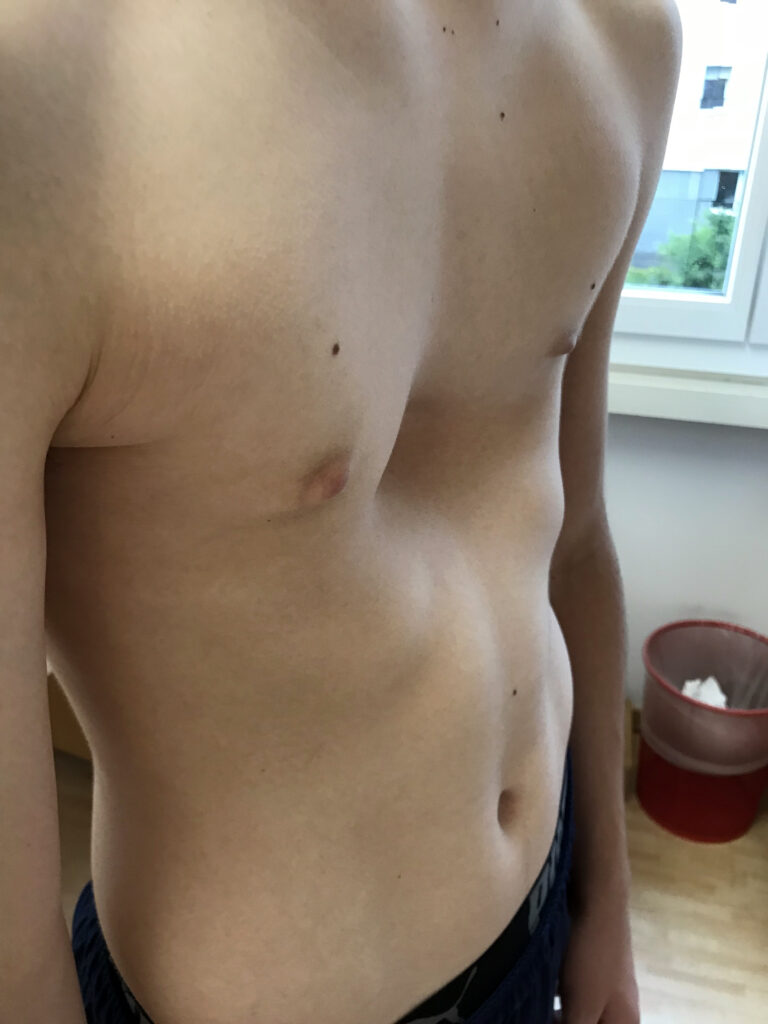
| Symptom Cluster: Pectus Excavatum | Clinical Presentation and Mechanism |
|---|---|
| Exercise Intolerance | Reduced cardiac filling leads to decreased stamina during sports. |
| Cardiac Dysrhythmias | Heart palpitations or irregular rhythms due to physical compression. |
| Respiratory Distress | Shallow breathing and chest tightness during physical exertion. |
| Postural Abnormalities | “Pectus posture”: hooked shoulders, thoracic kyphosis, protuberant abdomen. |
| Nutritional Stunting | Body burns extra calories at rest; patients often have difficulty gaining muscle. |
The phenomenon of the “pectus posture” is a critical second-order insight. Patients often subconsciously adopt a rounded-shoulder, slouched posture to hide the depression in their chest. Unfortunately, this posture further collapses the chest wall, potentially worsening the deformity and contributing to chronic back pain and spinal issues like scoliosis, which is associated with pectus in approximately 15% of cases.
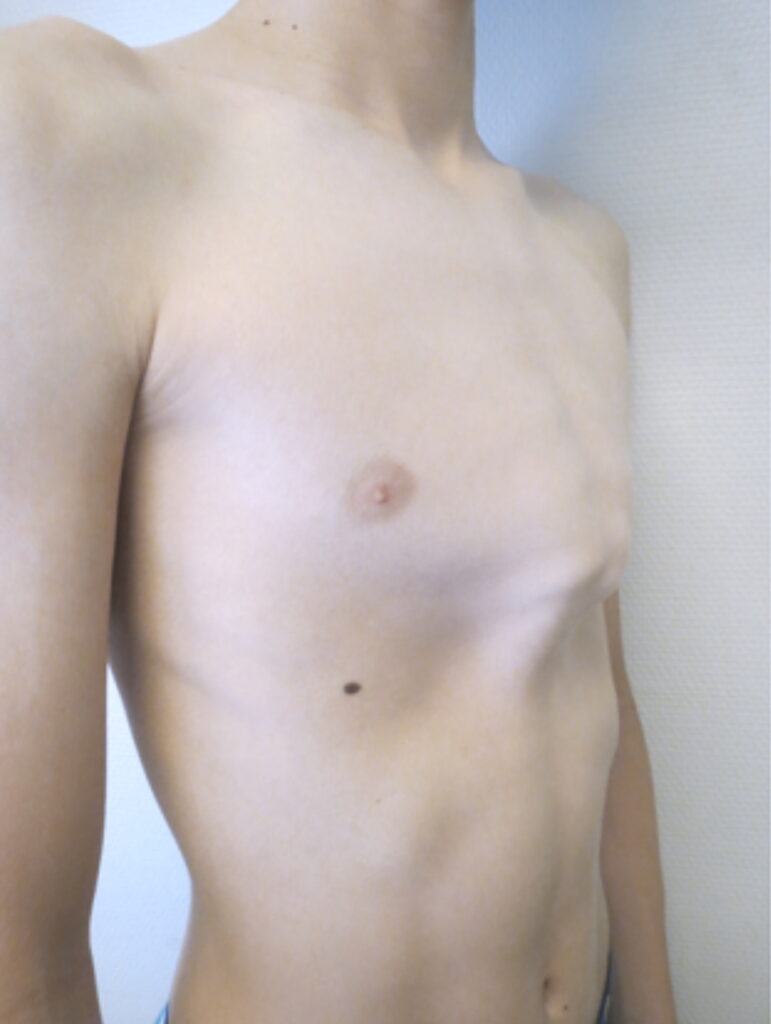
While pectus excavatum is characterized by its internal pressure, pectus carinatum presents as a visible external protrusion. Often referred to as “pigeon chest,” the condition causes the ribs and breastbone to grow outward, creating a birdlike appearance. Although it rarely compresses the heart to the same degree as excavatum, it is far from benign.
Patients with pectus carinatum frequently report thoracic pain, particularly when lying in a prone position or during contact sports. Furthermore, the protruding sternum can create a “barrel chest” configuration, which alters the normal mechanics of the chest wall. This can lead to inefficient breathing patterns and a sensation of breathlessness, sometimes misdiagnosed as asthma in up to a quarter of affected teenagers.
The psychological impact of pectus carinatum is often more acute because the deformity is harder to hide under clothing. Unlike a sunken chest, which can be obscured by a loose shirt, a protruding chest is frequently visible, leading to heightened self-consciousness and social anxiety during the sensitive years of puberty.
A formal diagnosis of a chest wall deformity begins with a detailed physical examination by a specialist like Dr. Schewitz, who assesses the symmetry, depth, and flexibility of the chest. However, clinical evaluation alone is insufficient to determine the need for surgical intervention. Advanced imaging and physiological testing are required to understand the impact on internal organs.
One of the primary metrics used in thoracic surgery is the Haller Index, calculated via CT or MRI scans. The index is a ratio of the horizontal width of the ribcage to the shortest distance between the sternum and the spine. A “normal” index is approximately 2.5, whereas an index greater than 3.2 is typically considered severe and may qualify as a medical indication for surgical repair.
| Diagnostic Test | Purpose and Clinical Value |
|---|---|
| CT / MRI Scan | To calculate the Haller Index and assess internal organ compression. |
| Echocardiogram | To evaluate heart function and detect mitral valve prolapse or displacement. |
| Pulmonary Function (PFT) | To measure lung capacity and identify restrictive breathing patterns. |
| 3D White Light Scanning | A radiation-free way to monitor the external shape of the chest over time. |
| Cardiopulmonary Exercise Test | To measure oxygen uptake and heart response during physical stress. |
The integration of these tests allows the thoracic surgeon to create a personalized treatment plan. In many cases, patients who appear “asymptomatic” are found to have significantly compromised heart or lung function when subjected to stress testing, highlighting the importance of a comprehensive diagnostic workup.
For decades, the standard treatment for chest wall deformities was the Ravitch procedure, a radical open surgery involving large incisions, the removal of costal cartilage, and the fracturing of the sternum to reposition it. While effective, the Ravitch procedure is associated with significant scarring, long recovery times, and the potential for the chest wall to become excessively rigid.
The paradigm shifted in the late 1980s when Dr. Donald Nuss developed the Minimally Invasive Repair of Pectus Excavatum (MIRPE), now known globally as the Nuss procedure. Dr. Schewitz, recognizing the transformative potential of this technique, was the first to perform it in South Africa, marking a new era for local pediatric patients.
The Nuss procedure involves the insertion of one or more customized stainless-steel bars behind the sternum through small incisions on the sides of the chest. Guided by a thoracoscope (a small camera), the surgeon positions the bar in a concave orientation and then rotates it 180 degrees. This rotation effectively “pops” the sunken sternum forward into a normal position, capitalizing on the natural flexibility of the adolescent ribcage.
The bars are secured to the ribs and remain in the body for approximately 3 years while the chest wall reshapes and the cartilage hardens in the new position. Once the correction is stable, the bars are removed in a simple follow-up procedure.
| Comparison Metric | Nuss Procedure (Minimally Invasive) | Ravitch Procedure (Open) |
|---|---|---|
| Primary Indication | Flexible chests (Adolescents) | Rigid or complex chests (Adults) |
| Incision Type | Two 2 cm lateral incisions | One large central incision |
| Tissue Resection | No cartilage or bone removed | Resection of costal cartilages |
| Operating Time | Typically under one hour | Significantly longer / more complex |
| Hospital Recovery | 2 to 3 days; high initial pain | 2 to 3 days; moderate pain |
| Cosmetic Outcome | Minimal scarring; immediate results | Visible scarring; gradual reshaping |
Despite its minimally invasive nature, the Nuss procedure is a major operation that requires sophisticated pain management, often involving epidural analgesia or cryotherapy to numb the nerves of the chest wall. Dr. Schewitz’s expertise in these postoperative protocols has been instrumental in reducing the recovery burden for South African families.
Not every chest wall deformity requires surgery. For many parents, the prospect of an operation is daunting, and for children with milder cases, non-surgical alternatives offer a viable path to correction, provided they are initiated during the “goldilocks” window of chest wall flexibility
For pectus carinatum, external bracing is now the gold standard of care. The technique utilizes a custom-fitted, low-profile aluminum brace that applies constant pressure to the protruding sternum. Much like orthodontic braces for teeth, the chest brace gradually reshapes the cartilage over a period of 12 to 24 months.
A major innovation in this area is Dr. Schewitz’s move toward 3D-printed braces in South Africa. By utilizing local manufacturing and precise 3D imaging, these braces are not only more comfortable and effective but are also significantly more affordable than imported models, which can be prohibitively expensive for South African families.
For mild to moderate pectus excavatum, the vacuum bell offers a non-invasive lifting mechanism. This device creates a suction seal over the depression, physically pulling the sternum forward. While it can produce an immediate elevation, long-term success requires extreme patient motivation, as the device must be worn for several hours every day for a minimum of two years. This therapy is most effective in younger children whose chest walls have not yet begun to stiffen.
The psychological weight of a chest wall deformity is often the primary reason parents seek Dr. Schewitz’s help. Adolescence is a period of intense focus on physical appearance and social belonging. A child with a visible chest anomaly may experience profound feelings of embarrassment and “otherness,” leading to social withdrawal and a refusal to participate in activities where their chest might be exposed, such as swimming or gym classes.
Studies have shown that even mild cases of pectus can lead to clinical depression and anxiety in teenagers. For many, the deformity feels like a “lonely road,” especially when medical professionals dismiss their concerns as purely aesthetic. Dr. Schewitz has frequently noted that the “instant” correction provided by the Nuss procedure often leads to a dramatic boost in self-esteem, with patients describing a sense of freedom and confidence they had never previously experienced.
In South Africa, the intersection of pectus deformities and contact sports, specifically rugby, is a frequent point of discussion. Many parents worry that a sunken chest makes their child more vulnerable to injury or that surgery will end their child’s athletic aspirations.
Contrary to these fears, the correction of pectus excavatum often enables a child to reach their full athletic potential. By relieving the pressure on the heart and lungs, surgery can increase stamina and oxygenation, allowing children who previously struggled to keep up with their peers to excel in competitive sports.
| Sport Consideration | Impact of Deformity | Post-Surgical Recovery (Nuss) |
|---|---|---|
| Rugby / Contact Sports | Risk of chest trauma; reduced stamina. | Full contact is usually allowed after 6–12 months. |
| Swimming | Often avoided due to body image issues. | Excellent for recovery; usually resume early. |
| Gym / Weightlifting | Limited by fatigue and poor posture. | Encouraged after 3 months to build muscle. |
| Aerobic Sports (Soccer) | Restricted by reduced cardiac output. | Significant improvement in endurance. |
The Nuss procedure is particularly well-suited for athletes because the chest wall remains structurally intact. Once the bars are secure and the initial healing is complete, the chest is actually reinforced by the steel bars, which can provide a degree of protection during the period they are in place. Dr. Schewitz has treated numerous patients who have gone on to represent their provinces and even become professional athletes following their recovery.
The financial and logistical reality of treating a chest wall deformity in South Africa involves navigating the complex world of medical aid and private hospital costs. Despite the clear physiological evidence of heart and lung impairment, many medical schemes in South Africa still attempt to classify pectus surgery as “cosmetic” or “non-essential”.
Discovery Health and other major schemes often require extensive motivation from a specialist like Dr. Schewitz to authorize the Nuss or Ravitch procedures. If a patient has a Haller Index above 3.2 or documented cardiac displacement, the procedure is more likely to be covered. However, even with approval, parents may face significant co-payments if they use specialists or hospitals outside of their scheme’s preferred network.
| Healthcare Cost Element | Estimated Range / Regulation (South Africa) |
|---|---|
| Initial Consultation | Variable; often requires specialist referral. |
| Private Hospital Day Rate | R4,700 to R5,700 (General Ward). |
| ICU / High Care Rate | R11,000 to R23,000 per day. |
| Nuss Hospital Costs | ~R150,000 (Case-specific pro bono example). |
| International Nuss Cost | ~R1,000,000 (For comparison with US-based care). |
| Discovery Health Rate | Cover at 100%, 200%, or 300% depending on plan. |
Ongoing need for advocacy and education within the insurance industry regarding the true nature of thoracic anomalies.
The success of Dr. Schewitz’s practice is best measured through the lived experiences of his patients. These stories reflect a common theme: a long period of uncertainty followed by a transformative intervention.
The case story illustrates the “silent” symptoms of pectus excavatum. For years, her shortness of breath and dizziness were dismissed as acid reflux or anxiety. It was only during her first pregnancy that the severity of her chest wall deformity was recognized, as the growing baby pushed her diaphragm up, further compressing her heart and leaving her bedbound. After consulting Dr. Schewitz and undergoing the Nuss procedure, even while pregnant with her second child, she experienced an immediate resolution of her symptoms. She was able to live an active life, gardening up until the birth of her third child, a feat that would have been impossible without surgical correction.
For younger patients like Johan, the intervention was as much about reclaiming their teenage years as it was about physical health. These patients, common in the South African school system, often transition from being the “quiet” or “withdrawn” student to being provincial representatives in sports or arts once the physical and psychological weight of the deformity is removed.
The future of pectus care in South Africa is inextricably linked to the continued advancement of minimally invasive technology and localized medical manufacturing. Dr. Schewitz’s work with 3D-printed braces and his leadership in the Chest Wall International Group ensure that South African children receive care that is at the cutting edge of global medicine.
As awareness grows, the goal is to shift the standard of care toward earlier detection and intervention. When parents and pediatricians recognize the early signs of an “inflated” or “deflated” chest, they can engage with experts while the chest wall is at its most malleable. This proactive approach minimizes the need for radical surgery and maximizes the physiological and psychological health of the next generation.
Based on the exhaustive research and clinical data provided by Dr. Ivan Schewitz and international thoracic bodies, the following recommendations serve as a guide for concerned parents:
The work of Dr. Ivan Schewitz at Netcare Waterfall City Hospital represents a beacon of hope for thousands of South African families. By combining pioneering surgical techniques with a deep understanding of the adolescent experience, the Pectus Clinic continues to transform lives, one chest wall at a time. The transition from a “sunken” or “pigeon” chest to a normal, healthy configuration is not just a medical procedure; it is the restoration of a child’s ability to breathe, play, and thrive in the world.
capetimes.co.za, pectusclinic.com, scribd.com, pacificcoastpediatricsurgery.com, pectuslab.com, researchgate.net, montrealchildrenshospital.ca, pectusclinic.com, med.umkc.edu, pectusweb.com, netcare.co.za, springboks.rugby, lemon8-app.com, discovery.co.za, hr.uct.ac.za
Contact Us – Dr. Ivan Schewitz, Cardiothoracic Surgeon
Doctor’s invention brings hope to three men – Pectus Clinic
Sellers’ Midwifery | PDF – Scribd
pacificcoastpediatricsurgery.com
Pediatric Chest Wall Deformities: When to Seek Surgery
A GUIDE TO PECTUS EXCAVATUM & CARINATUM | Montreal Children’s Hospital
Nuss Procedure | Pectus Clinic
Building on success – UMKC School of Medicine
Dynamic compression system for the correction of pectus carinatum – PectusWeb
It was the loneliest road I’ve ever walked… – Netcare
FRONT PAGE HEADING EVIDENCE-BASED LITERATURE REVIEW SAFE RUGBY TECHNIQUES
Understanding Pectus Excavatum: My Journey with Funnel Chest Surgery – Lemon8
The Comprehensive Series | Medical Aid Plans – Discovery
The Core Series | Hospital Plans| Medical Aid – Discovery
Discovery Health Medical Scheme
COVER FOR IN-ROOM PROCEDURES – Discovery
MCSA Private Tariff Schedule (South Africa) – 1 Jan 2024.xlsx